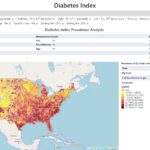
Eliminating Racial/Ethnic Disparities in Health Care: What are the Options?

Kaiser Family Foundation
Racial and ethnic disparities in health care – whether in insurance coverage, access, or quality of care – are one of many factors producing inequalities in health status in the United States.1 Eliminating these disparities is politically sensitive and challenging in part because their causes are intertwined with a contentious history of race relations in America. Nonetheless, assuring greater equity and accountability of the health care system is important to a growing constituency base, including health plan purchasers, payers, and providers of care. To the extent that inequities in the health care system result in lost productivity or use of services at a later stage of illness, there are health and social costs that affect us all.
Why Health Care Disparities Are a Concern
One in three residents of the United States self-identify as either African American, American Indian/Alaska Native, Asian, Native Hawaiian/Pacific Islander, Hispanic/Latino, or multiracial. By 2050, this number is expected to increase to one in two.2
Despite significant advances in civil rights, race remains a significant factor in determining whether an individual receives care, whether an individual receives high-quality care, and in determining health outcomes.
The Institute of Medicine (IOM) landmark report, Unequal Treatment, provides compelling evidence that racial/ethnic disparities persist in medical care for a number of health conditions and services.3 Numerous efforts are underway to reduce or eliminate racial and ethnic health care disparities, and to address some of the social factors that affect health care outcomes. Yet despite these many efforts, disparities in access to quality care remain, and for some measures being tracked, gaps in care are getting larger rather than smaller.4
Key Facts on Race, Ethnicity and Health Care in the U.S.
- Racial/ethnic disparities in health persist today even when comparing groups of similar SES. For example, the infant mortality rate for college-educated Black women is higher than that for White women with similar education (11.5 vs. 4.2 per 1,000 live births).
- The rate of new AIDS cases in 2003 was 3 times higher among Hispanics and 10 times higher among African Americans than among Whites (26 and 75 per 100,000 vs. 7 per 100,000).
- At least 1 in 3 nonelderly Latinos (36%) and AI/ANs (33%) is uninsured, as compared with 22% of African Americans, 17% of Asian and Pacific Islanders, and 13% of Whites.
- Insurance matters, as evidence by the fact that uninsured adults across racial/ethnic groups are at least twice as likely to go without a doctor visit in the past year.
- Black and Latino adults are less likely to rely on a private physician for their medical care than White adults (62% and 44% vs. 77%).
- African American children have a rate of hospitalization for asthma that is 4 to 5 times higher than the rate for White children (527 per 100,000 vs. 144 per 100,000).
- Disparities in quality of care are not getting smaller. Over time, the gap between Whites and African Americans, Hispanics, Asians, and AI/ANs has either remained the same or worsened for more than half of the core quality measures being tracked.
ADDRESSING HEALTH CARE DISPARITIES
Although attention to racial/ethnic disparities in care has increased among policymakers, there is little consensus on what can or should be done to reduce these disparities. The U.S. Congress provided early leadership on the issue by legislatively mandating the IOM study on health care disparities, creating the National Center on Minority Health and Health Disparities at the National Institutes of Health, and requiring DHHS to produce the National Healthcare Disparities Report.5 This brief examines four broad policy areas for addressing racial and ethnic health care disparities: READ FULL ARTICLE